Pharmacogenetics: An Introduction
BioCertica Content TeamWithin personalized medicine, genetic applications aid modern medicine in moving beyond the "one size fits all" treatment plan that is currently a norm in most healthcare systems. A major segment of personalized medicine is pharmacogenetics testing, which has significant implications for improving treatment plans by choosing the optimal treatment plan and avoiding adverse drug events (ADEs).
What is pharmacogenetics?
As you may know, your genetics essentially determine a range of factors, from your height to athletic ability. However, did you also know that they can influence how you respond to medication? Well, this is precisely where pharmacogenetics comes into play.
Pharmacogenetics is focused on understanding how variations present in the genome affect drug response. It has a major role in personalized medicine, a medical approach that tailors treatment and diagnostics to fit an individual or group of individuals.
Pharmacogenetics testing is becoming crucial in standard care, expanding to more drugs in the future[1]. Genetics can refine treatment, reducing drug toxicity and ADE risk. By avoiding trial and error, pharmacogenetics speeds up and cheapens the search for the best treatment plan[2].
How does pharmacogenetics work?
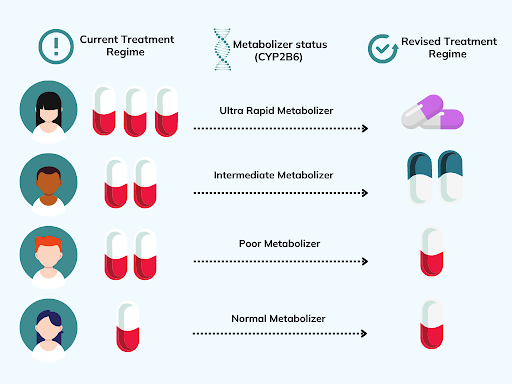
Your DNA acts as instructions to make proteins such as enzymes. Of particular interest for pharmacogenetics are the enzymes that metabolize drugs. There is a wide range of these enzymes, and a particular drug is typically only processed by one of these enzymes. Slight variations in the genes of these enzymes can alter how effective they are in processing pharmaceuticals and other substances. Sometimes it makes the enzyme less effective, resulting in the characteristic (phenotype) poor metabolizers.
This means that any drugs that are metabolized by this particular enzyme will likely be metabolized at a slower rate which could lead to the drug accumulating and building up in the system, and likely this will cause side effects. On the other hand, some genetic variants cause the enzyme to function almost too well and this means that the drugs may get processed too quickly and not have a chance to treat the issue.

Why do a pharmacogenetic test?
Say we have four people taking the same chronic medication but in varying dosages. Person A and person B both experience rather severe side effects from these drugs and therefore decide to do a pharmacogenetic test. Based on their results, they both realize that the current drug that they have been taking is not best suited to them as they metabolize it too quickly for it to be effective. One option would be to increase the dosage further but this could put too much strain on the liver. The better option would to find alternative drugs that are metabolized by a different enzyme.
Person C experiences some side effects from this drug because he is a poor metabolizer, which means the drug stays in his system for longer. Therefore adjusting the dosage will minimize his side effects.
Person D likely does not experience side effects and should continue with her current regime as it is likely best suited to her.

Benefits of pharmacogenetic testing
The two greatest benefits of pharmacogenetic test are of course giving you a plan for the most effective treatment while minimizing the risk of side effects. Without finding a pharmacogenetic test, getting to the most optimal treatment would be a long trial-and-error process that would be costly and prolong a decreased quality of life [3].

Pharmacogenetics is becoming a fundamental part of the future of medicine. Not too far into the future, it will be common practice to walk into a doctor's office with a pharmacogenetic test in hand and leave with a personalized treatment plan. This is the key to an improved quality of life for patients in general.
*Disclaimer:
The term “drug” in the above article refers to a chemical substance used to treat, cure, diagnose or prevent a disease or condition. Alternatives for this term include medication, pharmaceutical or therapeutic agents. In this context, “drug” does not refer to any type of illegal stimulant or recreational drug.
References
[1] J. P. Kitzmiller, D. K. Groen, M. A. Phelps, and W. Sadee, “Pharmacogenomic testing: Relevance in medical practice. Cleveland Clinic Journal of Medicine, vol. 78, no. 4. NIH Public Access, pp. 243–257, Apr-2011.
[2] D. B. Singh, “The Impact of Pharmacogenomics in Personalized Medicine,” in Advances in Biochemical Engineering/Biotechnology, vol. 171, Springer, 2020, pp. 369–394.
[3] A. T. Amare, K. O. Schubert, and B. T. Baune, “Pharmacogenomics in the treatment of mood disorders: Strategies and Opportunities for personalized psychiatry,” EPMA Journal, vol. 8, no. 3. Springer International Publishing, pp. 211–227, 05-Sep-2017.
Interested in trying the BioCertica Pharmacogenetics DNA kit? Click here and add Pharmacogenetics to your cart for only R3099.
If you own any other BioCertica DNA kit, you can instantly unlock your Pharmacogenetics results for only R1999* in-app.
*Terms and conditions apply.
Written by: Jamie Fernandez, B.Sc. Hons. in Genetics, Content Specialist
Peer-reviewed by: Edin Hamzić, Ph.D. in Genetics, Chief Science Officer



